The number of total hip replacement (THR) is constantly increasing with currently around 150,000 prosthesis implanted each year in France. At the same time, the indications for THR have widened, which has had the effect of rejuvenating the population of operated patients. As a result, questions regarding sexual activity after a THR have become more and more frequent even though the majority of patients still do not dare to discuss this topic with their surgeon, possibly out of timidity or embarrassment.
Sexual activity is of course possible after a THR and it is also most often improved by the operation because hip pathologies are often responsible for pain during sexual intercourse.
It is legitimate to be apprehensive about resuming a normal sex life after the operation because you have to “tame” your new hip. Fortunately, there are very few risks involved in having sex after a THR.
The main risk is the dislocation of the prosthesis. It is especially present during the first 3 postoperative months while the tissue healing around the prosthesis takes place and the muscles regain satisfactory tone.
This risk of dislocation depends on several factors:
- The surgical approach by which the THR was performed. It is especially the posterior approach that causes a risk of early dislocation due to the tendon section performed by this technique which decreases the natural coaptation of the joint during the first postoperative months. On the other hand, it has been shown that the risk of dislocation after an anterior Hueter approach, which preserves the muscles and tendons, was markedly reduced compared to the posterior approaches.
- The orientation of the prosthesis implants: during specific movements of great amplitude, abnormal contact between the acetabular implant (of the pelvis) and the prosthetic femoral stem may occur, risking dislocation. This contact can be facilitated by certain variations in the orientation of prosthetic implants.
- The position or positions adopted during intercourse, themselves dependent on the sex of the patient, may, in some cases, favor the occurrence of a dislocation.
All this was carefully analyzed by a Swiss team which, in 2013, published a study on 12 positions frequently encountered during sexual intercourse. After carrying out a kinematic analysis by optical sensors of the position in space of the pelvis and the femur of the 2 partners in these 12 positions, the authors extrapolated using a computer simulation what the position of the implants of the prosthesis in these same positions and deduced which were the positions at risk of dislocation and which were the “safe” positions, making the distinction according to whether the operated was a man or a woman.
The following diagram provides you with a summary of the findings of this article. It is to highlight that :
- The female positions at risk of dislocation (n ° 3,5,8,10) are more numerous than for the male positions (n° 8).
- Female positions only entail a risk of posterior dislocation, the occurrence of which is exceptional in the event of a TRH performed by an anterior approach.
- The only male position described considered to be at risk (n ° 8), entails a risk of anterior dislocation.
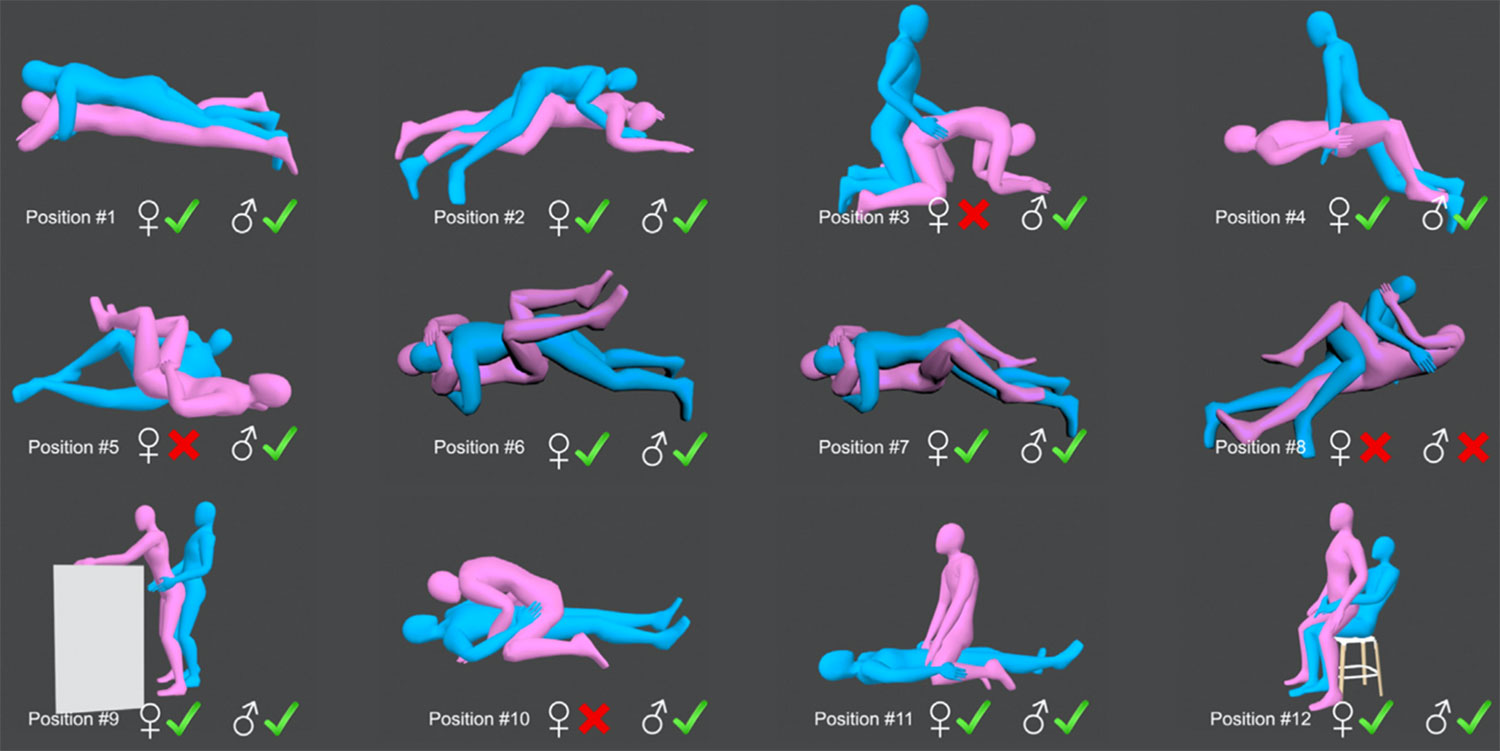
In summary, sexual activity can be resumed early after the operation as soon as the patient feels able to do so, but it is preferable to avoid certain positions during the first 3 months, especially since the THR was performed by a posterior approach which is more at risk of dislocations than the Hueter anterior approach.
Discover the operation linked to this article:
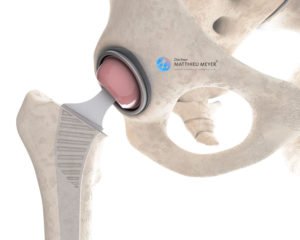
Minimally Invasive Anterior Approach Total Hip Replacement
Some pathologies such as hip osteoarthritis or necrosis of the femoral head can require a total hip replacement. A minimally invasive anterior approach can be used for this arthroplasty, which spares all the muscles and tendons thus enabling faster recovery and reducing the risk of dislocation of the prosthesis.

